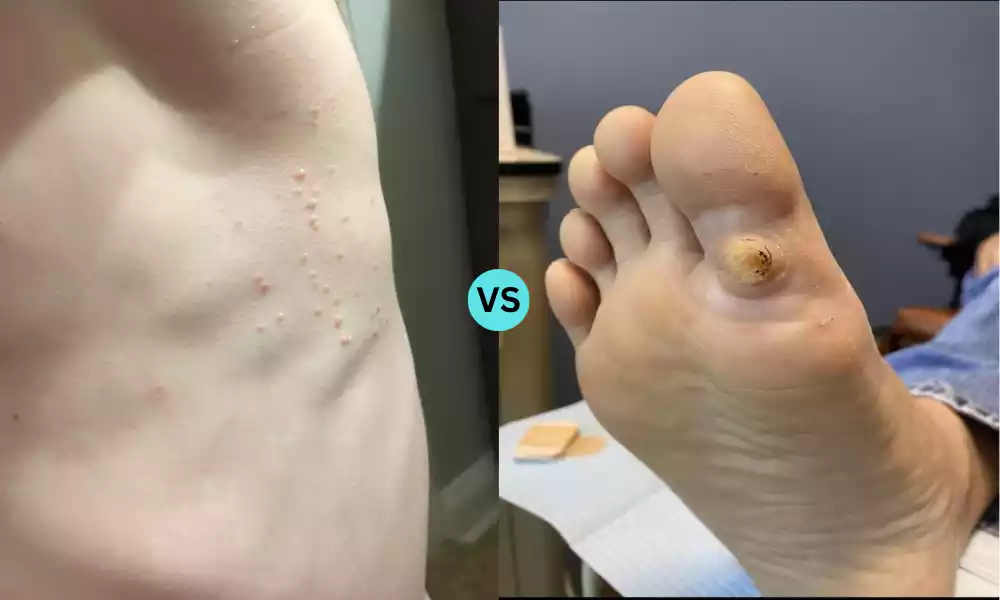
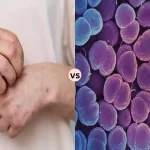
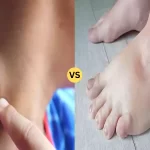
Molluscum Contagiosum and Warts are both common skin infections caused by viruses. Molluscum contagiosum is triggered by the molluscum contagiosum virus, leading to small, painless, raised lesions with a central dimple. It is especially prevalent among children and is spread through direct skin-to-skin contact or contact with contaminated objects.
Warts, on the other hand, are caused by various strains of the human papillomavirus (HPV) and can appear on any part of the body. They present as rough, raised bumps and can vary in size and appearance. Both conditions are generally harmless, but can be bothersome or unsightly, and may spread to other parts of the body or to other people.
What is Molluscum Contagiosum?
Molluscum contagiosum is a skin infection caused by the molluscum contagiosum virus. It is characterized by small, raised, pearl-like nodules or papules on the skin, often with a central dimple. These lesions can appear anywhere on the body but are commonly found on the face, neck, arms, and legs. The condition is most prevalent in children, though it can affect individuals of any age.

Transmission typically occurs through direct skin-to-skin contact or by touching contaminated objects. While the infection is generally benign and self-limiting, it can be spread to other areas of the body or to other individuals.
Causes of Molluscum Contagiosum
Molluscum contagiosum is caused by the molluscum contagiosum virus (MCV), a member of the poxvirus family. The transmission of this virus can occur in various ways:
- Direct Skin-to-Skin Contact: The most common mode of transmission is through direct contact with the skin of an infected person.
- Contaminated Objects: The virus can be spread by touching objects that have been contaminated with the virus, such as towels, clothing, toys, or sports equipment.
- Sexual Transmission: In adults, molluscum contagiosum can be sexually transmitted if the lesions are present in the genital area.
- Autoinoculation: This is the self-transfer of the virus from one part of the body to another, often via scratching or touching a lesion and then another part of the body.
- Water Sources: There are reports of transmission in swimming pools or shared baths, although the risk is considered low. The moist environment can help the virus survive and possibly aid in its transmission, especially if there’s close skin-to-skin contact.
- Shared Personal Items: Using personal items like razors, brushes, or other grooming tools of someone with the infection can lead to transmission.
- Close Environments: Outbreaks have been reported in settings where people are in close contact with one another, such as in daycare centers or schools.
It’s essential to maintain proper hygiene and avoid direct contact with lesions to prevent the spread of molluscum contagiosum. If someone suspects they have the condition, it’s advisable to see a healthcare professional for diagnosis and guidance on management.
Symptoms of Molluscum Contagiosum
Molluscum contagiosum presents with distinctive skin lesions that have several characteristic features:
- Raised Bumps (Papules): The primary symptom is the appearance of small, raised, flesh-colored or pinkish-white bumps (papules) on the skin.
- Central Dimple: These papules often have a characteristic central dimple or indentation.
- Smooth and Firm Texture: The bumps are typically smooth, firm, and dome-shaped.
- Size: The lesions are usually small, ranging from about the size of a pinhead to as large as a pencil eraser (2 to 5 millimeters in diameter).
- Painless: While the lesions are generally painless, they can become itchy or tender.
- Content: If squeezed, the bumps can release a thick, waxy core which contains the virus.
- Location: They can appear anywhere on the body but are most common on the face, neck, armpits, arms, and hands. In adults, they can also be found in the genital area, indicating a possible sexual transmission.
- Number: An individual may have just one or a few papules, or they might have dozens spread across the body.
- Duration: Without treatment, the bumps typically last from several months to a few years. However, they will eventually go away on their own.
- Secondary Infections: Scratching or picking at the lesions can lead to bacterial infections, which might result in redness, swelling, pain, and pus.
As this can lead to spreading them to other parts of the body or to other individuals. If someone suspects they have molluscum contagiosum, they should consult a healthcare professional for a proper diagnosis and advice on management.
What are Warts?
Warts are small, benign growths on the skin caused by various strains of the human papillomavirus (HPV). They can appear anywhere on the body and manifest in different forms, such as common warts, flat warts, plantar warts, and filiform warts. The appearance of a wart can vary from rough, raised bumps to flat or thread-like structures, depending on its type and location.
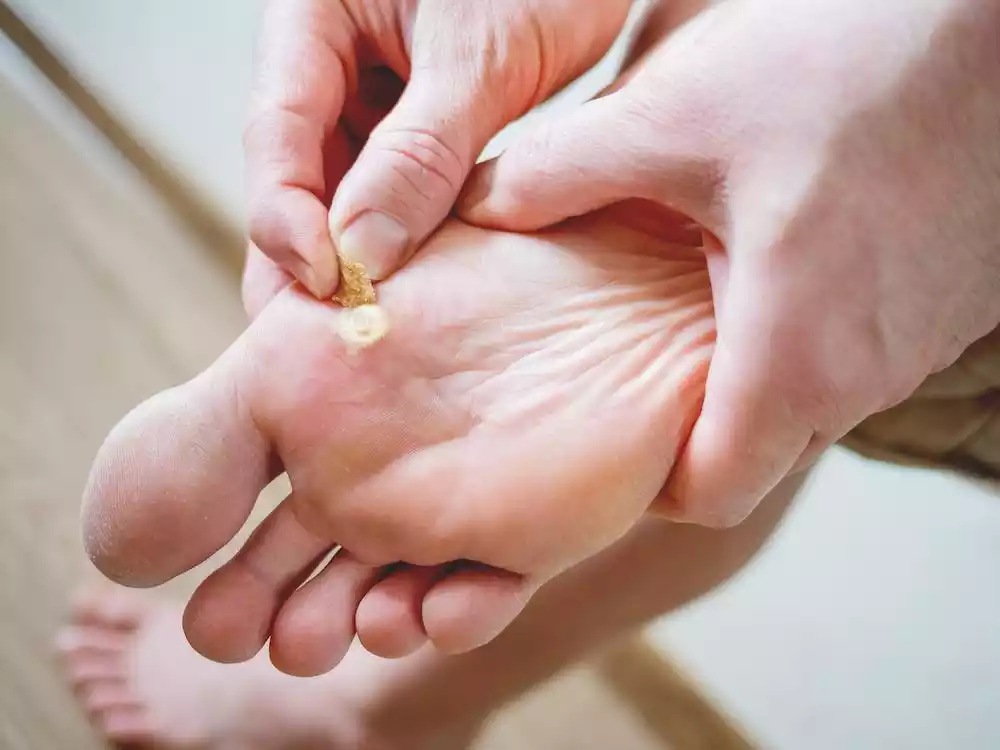
Warts are contagious and can spread through direct skin-to-skin contact or by touching surfaces that an infected person has come into contact with. While warts are usually harmless, they can be bothersome or unsightly, and some individuals may seek treatment for their removal.
Causes of Warts
Warts are caused by the human papillomavirus (HPV), a diverse group of viruses with over 100 different types. Different types of HPVs are responsible for different types of warts. The transmission of this virus can occur in various ways:
- Direct Skin-to-Skin Contact: Coming into direct contact with a wart on another person can lead to transmission.
- Autoinoculation: This refers to the transfer of the virus from one part of an individual’s body to another, often through scratching or touching a wart and then touching another part of the body.
- Contaminated Surfaces: Walking barefoot in public places, such as locker rooms, showers, or pool areas, can expose one to strains of HPV that cause plantar warts. The virus thrives in warm, moist environments.
- Shared Personal Items: Using personal items that have been used by someone with a wart, such as towels, razors, or shoes, can lead to transmission.
- Minor Skin Trauma: The virus can enter the body through small cuts, scrapes, or breaks in the skin. This is one reason why areas of the skin that are frequently shaved (like the legs) or bitten (like the nails) may be more susceptible to warts.
- Close Environments: Settings where people are in close contact with one another, such as schools or communal living situations, can facilitate the spread of warts.
HPV will develop warts, as the immune system plays a significant role in determining susceptibility. Some people are naturally more resistant, while others might be more prone to developing warts when exposed to the virus.
To minimize the risk of getting or spreading warts, it’s essential to maintain proper hygiene, avoid direct contact with warts, and avoid sharing personal items. If someone suspects they have warts, they should consult a healthcare professional for proper diagnosis and treatment.
Symptoms of Warts
Warts are skin growths caused by the human papillomavirus (HPV). Their appearance and symptoms can vary depending on the type of wart and its location. Here are the general and specific symptoms associated with common types of warts:
- Common Warts:
- Raised growths with a rough surface.
- Typically appear on the hands but can develop elsewhere.
- May have black pinpoints, which are clotted blood vessels.
- Plantar Warts (found on the soles of the feet):
- Hard, thick patches of skin, often with a callus over the top.
- Can be painful when walking or standing, feeling like pebbles in the shoe.
- May have black pinpoints.
- Flat Warts:
- Smaller, flat-topped lesions.
- Smooth and can be pink, light brown, or yellowish.
- Often appear in large numbers.
- Commonly found on the face, arms, and legs.
- Filiform Warts:
- Long, thread-like growths.
- Commonly appear on the face, especially around the eyes, mouth, and nose.
- Periungual Warts (around or under the nails):
- Rough growths that can affect nail growth.
- Can be painful.
- Genital Warts (a sexually transmitted form of wart):
- Soft growths that appear on the genitals.
- Can be raised or flat, single or in clusters.
- May cause itching or discomfort.
- Some strains associated with genital warts carry a higher risk of leading to certain types of cancers, but many strains do not.
General Characteristics:
- Most warts are painless unless they’re in areas of frequent pressure or friction.
- They might be flesh-colored, gray, brown, or white.
- Warts can spread through direct contact or indirectly through shared environments like showers or swimming pools.
- Some warts might itch.
If someone suspects they have a wart, especially a genital wart, it’s essential to consult a healthcare professional for an accurate diagnosis and advice on treatment.
Comparison table of Molluscum Contagiosum and Warts
Comparison of Molluscum Contagiosum and Warts:
| Features | Molluscum Contagiosum | Warts |
|---|---|---|
| Causative Agent | Molluscum contagiosum virus | Human papillomavirus (HPV) |
| Appearance | Small, shiny, firm bumps; can be pink, white, or skin-colored | Rough-textured growths, often with tiny black dots; can vary in size |
| Texture | Smooth and firm | Rough and grainy |
| Common Areas of Occurrence | Face, neck, arms, back of the hands | Fingers, hands, feet; can appear elsewhere too |
| Transmission | Direct skin-to-skin contact, contaminated objects | Direct skin-to-skin contact, scratches, and cuts, walking barefoot in public areas |
| Treatment Options | Over-the-counter creams, cryotherapy, laser therapy, curettage | Over-the-counter creams, cryotherapy, surgical removal, laser therapy |
| Natural Remedies | Apple cider vinegar, tea tree oil | Garlic, baking soda |
| Potential Complications | Secondary bacterial infections if scratched | Spread to other areas, can be painful (especially plantar warts) |
| Prevention | Avoid direct contact, don’t share personal items | Avoid walking barefoot, keep hands and feet dry, avoid direct contact |
| Duration | Can last from a few months to several years | Can last for months to years; may resolve on their own |
| Associated Stigma | Minimal (often confused with other skin conditions) | Some types, especially genital warts, can carry a stigma |
While this table provides a concise comparison, it’s always best to consult a dermatologist or a medical professional for any skin concerns or conditions.
Similarities between Molluscum Contagiosum and Warts
Molluscum contagiosum and warts share several similarities, including:
- Viral Origin: Both are caused by viruses. Molluscum contagiosum is caused by the molluscum contagiosum virus, while warts are caused by various strains of the human papillomavirus (HPV).
- Contagiousness: Both conditions are contagious and can spread through direct skin-to-skin contact. They can also spread by touching objects or surfaces that have been contaminated with the respective virus.
- Skin Growths: Both manifest as raised growths or lesions on the skin.
- Benign Nature: Both are generally benign conditions, meaning they are not cancerous and typically do not pose serious health risks.
- Can Affect Anyone: While certain populations may be more susceptible (e.g., molluscum is more common in children), both conditions can affect individuals of any age.
- Self-limiting: Many cases of both molluscum contagiosum and warts can resolve on their own without treatment, though this can take months to years.
- Treatment Options: Both can be treated using similar methods, such as cryotherapy (freezing). However, the choice of treatment might vary depending on the size, location, and number of lesions, as well as patient preference.
- Reoccurrence: Even after successful treatment, both molluscum contagiosum and warts can reappear, especially if the individual is re-exposed to the virus.
- Spread to Other Body Parts: Both conditions can spread to other areas of the same individual’s body through autoinoculation, which is the transfer of the virus from one part of the body to another.
Despite these similarities, the two conditions have distinct characteristics and should be diagnosed and treated appropriately. If someone suspects they have either condition, they should consult a healthcare professional or dermatologist.
Diagnosis and Testing of Molluscum Contagiosum and Warts
Molluscum Contagiosum:
Diagnosis
- Clinical Examination: Most often, the diagnosis of molluscum contagiosum is made based on the characteristic appearance of the lesions (small, raised, pearl-like nodules with a central dimple).
- Dermoscopy: Some dermatologists might use a dermoscope, a device that illuminates and magnifies skin structures, to examine the lesions more closely.
- Skin Biopsy: In unclear cases or when the lesions look atypical, a skin biopsy might be performed. In this procedure, a small sample of the lesion is removed and examined under a microscope to confirm the presence of the molluscum contagiosum virus.
Testing: There is no routine blood or imaging test for molluscum contagiosum. Diagnosis is primarily based on clinical observation and, if needed, biopsy.
Warts
Diagnosis:
- Clinical Examination: The diagnosis of warts is typically made based on their characteristic appearance, which varies depending on the type of wart (e.g., common, plantar, flat).
- Acetic Acid Application: In some cases, especially for genital warts, a weak acetic acid solution might be applied to the skin. This can make warts turn white and become more visible. However, this method is not specific, as other lesions can also turn white.
- Skin Biopsy: If there’s uncertainty about the diagnosis, or if a wart looks atypical, a skin biopsy might be conducted. The sample is then examined under a microscope to confirm the presence of the wart and rule out other conditions like skin cancer.
Testing:
- HPV Typing: While not routinely done for common warts, in certain situations (especially with genital warts), a test might be conducted to determine the specific strain of HPV causing the warts. This can be relevant because some HPV strains are associated with a higher risk of cancer.
- Other Tests: For genital warts, additional tests might be recommended to check for other sexually transmitted infections.
A trained healthcare professional or dermatologist can diagnose molluscum contagiosum and warts based on a simple physical examination. However, further tests might be necessary if there’s any doubt or if other conditions need to be ruled out. If someone suspects they have either condition, they should seek medical advice for a definitive diagnosis and appropriate management.
Treatment for Molluscum Contagiosum
Molluscum contagiosum is often a self-limiting condition, meaning it can resolve on its own without treatment. Treatment may be considered for various reasons, such as to hasten resolution, reduce the risk of spreading to others, or for cosmetic reasons.
Here are some common treatment options for molluscum contagiosum:
- Observation: Since many cases resolve without intervention, especially in children, a “wait and see” approach might be recommended. The bumps can last from a few months to a few years, but most cases clear up within a year.
- Cryotherapy: This is one of the most common treatments. Liquid nitrogen is applied to each bump, freezing and destroying the lesion. Multiple sessions might be needed.
- Curettage: The dermatologist uses a small, sharp instrument (a curette) to scrape off the bumps. Local anesthesia might be used to numb the area.
- Laser Therapy: A laser is used to destroy the lesions. This option might be considered for larger outbreaks or when other treatments fail.
- Topical Therapies: There are various creams, gels, and solutions that can be applied directly to the lesions to help them resolve. Some common ones include:
- Imiquimod cream: An immune response modifier that can help the body fight the virus.
- Podophyllotoxin cream: Derived from plants and works by poisoning the cells of the lesions.
- Salicylic acid: Can help remove the top layers of the bump.
- Potassium hydroxide: Causes the lesions to dissolve over time.
- Cantharidin: This is a blistering agent derived from the blister beetle. When applied to the bumps, it causes them to blister, and they can then be trimmed away. This treatment is often called “beetle juice.”
- Oral Medications: In severe cases, or when the patient has a weakened immune system, oral antiviral drugs might be prescribed.
- Avoid Scratching: While not a treatment per se, it’s crucial to avoid scratching or picking at the lesions, as this can cause them to spread to other parts of the body or lead to bacterial infections.
It’s essential to consult with a dermatologist or another healthcare professional before starting any treatment. They can help decide the best treatment option based on the patient’s age, health, the number and location of lesions, and other factors.
Treatment for Warts
Treatment for warts depends on their type, location, and severity, as well as the patient’s age, health status, and preferences. Here are some of the common treatment options for warts:
- Observation: Not all warts require treatment. Some may go away on their own, especially in children. This might take months or even years, but if the wart is not bothersome, waiting can be an option.
- Salicylic Acid: Available over-the-counter in various preparations (like patches, gels, and solutions), salicylic acid works by exfoliating the layers of the wart. It’s applied directly to the wart after soaking the area in warm water. This treatment is often used for common warts and plantar warts.
- Cryotherapy: A healthcare provider applies liquid nitrogen to freeze the wart, causing it to blister and eventually fall off. This method can cause some discomfort and may require multiple sessions.
- Curettage: Involves scraping off the wart with a curette, a sharp-edged instrument. It’s sometimes combined with electrosurgery (burning) for better efficacy.
- Laser Treatment: Pulsed-dye laser or carbon dioxide (CO2) lasers can be used to burn off the wart tissue. This treatment might cause pain and scarring and is generally reserved for warts that have not responded to other therapies.
- Chemical Treatments: A healthcare provider might apply various chemicals to destroy the wart tissue. Examples include cantharidin (often mixed with other compounds) or bleomycin.
- Imiquimod Cream: An immune response modifier primarily used for genital warts. It works by stimulating the body’s own defenses to fight off the wart virus.
- Duct Tape: There’s some evidence suggesting that covering the wart with strong adhesive tape (like duct tape) can help in its removal. The method involves covering the wart for about six days, soaking it in water, gently debriding it with an emery board or pumice stone, and then re-applying tape. This process is repeated for several weeks.
- Vaccination: The HPV vaccine, which is primarily designed to protect against cancer-causing strains of HPV, may also help in treating warts, especially genital warts.
- Oral Medications: In some resistant cases, oral medications like cimetidine or retinoids might be prescribed, although this is less common.
- Avoid Spreading: As with molluscum contagiosum, it’s crucial not to pick or scratch warts to prevent spreading them to other parts of the body or to other people.
Choosing the right treatment often depends on the patient’s preferences, pain tolerance, and the wart’s location and size. It’s essential to consult with a dermatologist or another healthcare professional to determine the best treatment strategy.
Potential Complications
Both molluscum contagiosum and warts are generally benign conditions, but they can lead to complications if not managed appropriately.
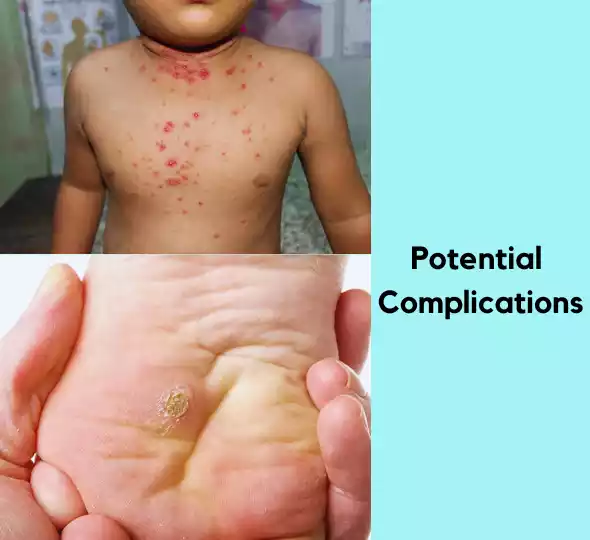
Here are potential complications for each:
Molluscum Contagiosum:
- Secondary Bacterial Infections: Scratching or picking at the lesions can cause them to become infected with bacteria. This can lead to the formation of pus, pain, swelling, and redness around the lesions.
- Scarring: If the lesions become inflamed, infected, or are scratched, they can leave scars once they heal.
- Spread to Other Areas: If an individual picks at or scratches the lesions, they can spread the virus to other parts of their body.
- Ongoing Spread to Others: Molluscum contagiosum is contagious. Without appropriate care or treatment, an individual can transmit it to other people.
- Inflammation and Redness: Some lesions can become inflamed, leading to redness and swelling.
- Eye Complications: If the virus affects the eyes, it can cause conjunctivitis or even keratitis.
Warts:
- Spread: Warts can spread to other parts of the body, especially if they are picked at or if the skin is broken.
- Reoccurrence: Even after treatment, warts can return.
- Scarring: Some treatments or the natural course of a wart can leave a scar.
- Pain: Some warts, especially plantar warts, can be painful. This pain can interfere with walking or other activities.
- Secondary Bacterial Infections: Just like with molluscum contagiosum, scratching or picking at warts can introduce bacteria, leading to infections.
- Malignant Transformation: Although extremely rare, some genital warts due to specific HPV strains can progress to cancer if not treated.
- Emotional Distress: Visible warts, especially on the face or hands, can lead to self-consciousness or embarrassment.
- Complications in Immune-compromised Individuals: People with weakened immune systems might have a harder time fighting off the HPV virus, leading to larger or more numerous warts.
Preventing these complications largely revolves around proper hygiene, not scratching or picking at lesions, and seeking appropriate medical treatment when necessary. If there are signs of complications, such as signs of infection or unusually persistent or painful lesions, it’s essential to consult a healthcare professional.
Prevention Tips
Preventing molluscum contagiosum and warts primarily involves minimizing exposure to the viruses that cause them. Here are some prevention tips for each:
Molluscum Contagiosum Prevention:
- Avoid Direct Contact: Since molluscum contagiosum spreads through skin-to-skin contact, avoid touching or being touched by someone’s lesions.
- Don’t Share Personal Items: Don’t share towels, clothing, or other personal items with someone who has molluscum contagiosum.
- Practice Good Hand Hygiene: Wash your hands regularly with soap and water.
- Keep Lesions Covered: If you or someone you know has molluscum contagiosum, keep the lesions covered with clothing or bandages to prevent spreading.
- Avoid Scratching: Scratching can spread the virus to other parts of the body.
- Avoid Shared Swimming Areas: If possible, avoid swimming pools, saunas, or other shared bathing areas if you or someone you’re with has active lesions.
- Sexual Contact: For adults, if the lesions are in the genital area, it’s best to abstain from sexual contact until the lesions are treated and have disappeared.
Warts Prevention:
- Avoid Direct Contact: Don’t touch someone else’s warts. This includes shaking hands if there’s an active wart on the hand.
- Wear Protective Footwear: In communal areas, like public showers or swimming pools, wear flip-flops or water shoes to avoid getting plantar warts.
- Don’t Pick or Bite: Avoid biting your nails or picking at hangnails, as warts can develop around nails.
- Keep Skin Healthy: Any cuts or scrapes should be cleaned and covered to prevent the HPV virus from entering the skin.
- Avoid Reusing or Sharing Items: Don’t use the same emery board, pumice stone, or nail clipper on a wart that you use on healthy skin and nails.
- Strengthen Immune System: A robust immune system can help fend off warts, so maintain a healthy lifestyle with a balanced diet, regular exercise, and adequate sleep.
- Safe Sex: Genital warts spread through sexual contact. Use protection (like condoms) and consider getting the HPV vaccine, which can protect against the most common strains of HPV that cause genital warts and cervical cancer.
- HPV Vaccination: Consider getting vaccinated. The vaccine protects against several strains of HPV, including those most likely to cause genital warts and cancers.
By following these tips and being aware of your environment, you can reduce the risk of contracting or spreading molluscum contagiosum and warts.
Conclusion
Molluscum contagiosum and warts are skin conditions caused by viral infections, specifically the molluscum contagiosum virus and the human papillomavirus (HPV), respectively. Both can present as raised lesions on the skin, but they differ in appearance, symptoms, and potential complications. While they are typically benign and self-limiting, they can be sources of discomfort, cosmetic concern, or potential spread to others.
Various treatments are available, ranging from topical applications to more invasive procedures, depending on the severity and location of the lesions. Prevention, focusing on hygiene and avoiding direct contact with infected areas, is crucial in managing and reducing the spread of these conditions.